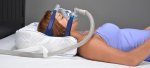
Suffering from aerophagia and mixed sleep apnea
by Michelle
(Wyoming )
I am a 44 year old female. I am 118 lbs and I live at 7100 feet. I lived 37 years at sea level.
The last three years I have been treated for Fibromyalgia, asthma and ADHD.
I felt like I was going to die, basically after a slow recovery from severe bronchitis last January.
In August I was diagnosed with mixed sleep apnea. It is moderate border line severe. More Central than obstructive.
Though I have been given a CPAP with permission to unhook the oxygen portion, at 9.0 CPAP pressure on a C-Flex machine with a mask that covers the nose only...
I have severe aerophagia.
I do have IBS (Irritable bowel syndrome), so maybe I am more sensitive.
I found research on GERD. About 10years ago I was diagnosed with that and stopped taking the medicine.
I am desperate for relief. I usually pull off CPAP after 2 hours because the pain from bloating and gas is too severe.
I sleep with the oxygen mask on just so I am not so tired the next day, I guess my brain is then getting oxygen but not the forced air into my stomach.
I have no idea why I have central sleep apnea.
Should I move down to a lower elevation, take GERD meds at night or ask for an antimuscarinic medication?
I am at my wits end and will probably flunk out of grad school. Had to reduce course load to one class.
Thanks for any suggestions in advance.
Michelle
Answer
Suffering from aerophagia is such a common issue in CPAP users that it should be included in every CPAP manual or discussed by every sleep doctor.
The gas pain happens when air enters the esophagus in to the stomach and causes bloating.
Aerophagia can be caused by eating or drinking too fast, by chewing gum, breathing too fast from anxiety or physical exercises, or smoking cigarettes.
In CPAP patients, the air enters from CPAP to esophagus and then in to the stomach rather than the airway and in to your lungs. This CPAP air will cause gas pain which can become chronic so it must be treated fast.
Causes of CPAP Aerophagia
Here are the most common risk factors for aerophagia in CPAP users:
- High CPAP air pressure - if you have a higher pressure than you require, the extra air has nowhere to enter, except in to your esophagus and stomach.
- Low CPAP air pressure - if the air pressure is too low, you will struggle to breathe air. In your effort to get more air in to your lungs, you can swallow air quickly that will be forced to enter in to the stomach.
- Nasal congestion - is one of the reasons where you get less air than necessary to breathe properly during sleep. So you'll swallow air that will go down in to the esophagus and stomach.
- Mouth breathing - if you use a nasal CPAP mask or nasal pillows, and if you are a mouth breather, the air that comes from CPAP may escape via your mouth instead entering the lungs.
By losing so much air, your body may suddenly have a choking sensation during sleep and you'll start swallowing air quickly, forcing it to the stomach. - Losing the natural rhythm of breathing - this can happen when you have difficulty adjusting to exhale over the constant pressure of the CPAP air.
Trying to exhale mostly against a higher CPAP air pressure may cause a feeling of suffocation. When this panic occurs, you can start breathe abnormally and hyperventilation may occur.
With hyperventilation, the same things happen: you'll start swallowing the air that will be forced in to the stomach rather than the airway and lungs.
By the way... Higher pressure than necessary will also cause central sleep apnea events. I'm wonder if you are in this situation...
Methods to Treat Aerophagia
Here are some tips to help you with Aerophagia:
- Check the CPAP pressure settings - if you think your CPAP air pressure is too high or too low, discuss with your doctor if he can change the pressure.
Moreover, investigate with your CPAP provider if your CPAP machine was set correctly as prescribed by your doctor. People are making mistakes, and maybe your CPAP was set incorrectly. - Check the quality of your CPAP mask - Did you make your best choice when you bought your CPAP mask?
There are some things to consider. For example, if you are a mouth breather but you're using a nasal mask, then you made the choice that will probably cause aerophagia.
Or, if you have mask leaks, this can also affect your breathing during the night. - Cognitive behavioral therapy - if you thing your aerophagia is caused by hyperventilation from panic attached or claustrophobic sensation, consider speaking with a sleep specialist about cognitive behavioral therapy for sleeping with a CPAP mask. He may also give you a referral to a psychologist.
Central Sleep Apnea and High Altitudes
Regarding to your central apnea episodes, some clinical studies demonstrated that people sleeping at high altitude have an increased risk of having central sleep apnea.
At altitudes higher than 5000 meters even if you breathe oxygen during that night, central events may appear. Read the study here.
Another study shows that patients with sleep apnea living at high altitudes (2.400 m) dropped their AHI from 53.8 to 33.1 when they traveled to sea level. Some of them had their AHI under 5/h at sea level so they didn't need therapy.
That's why a sleep study is more efficient if it's done where you live not at different altitudes.
The reduction of AHI was in fact a predominant reduction of central apneas and hypopneas episodes, and a slight reduction of obstructive apnea episodes. Read more about this study here.
Bottom line... I'm not surprised you have central apnea episodes when you live over 7000 feet. Some people have their breathing drive reflexes not calibrated to having so little oxygen in each breath of the thin air.
I think if you move to a lower altitude, with each breath you will inhale considerable more oxygen than now. At least, you should test sleeping at sea level and see what happens.
I hope it helps. Don't be afraid to comment back.
Remy Thierry
Founder of Sleep Apnea Guide
Comments for Suffering from aerophagia and mixed sleep apnea
|
||
|
||
|
||